An Objective Spatialomics Test Standardizes Management Decisions with Potential to Improve Outcomes for Barrett’s Esophagus Patients
Frei, Nicola F. F. MD1; Duits, Lucas C. MD, PhD2; Khoshiwal, Amir MD3; Pouw, Roos E. MD, PhD3; Smolko, Christian PhD4; Arora, Meenakshi PhD4; Siegel, Jennifer J. MA, PhD5; Critchley-Thorne, Rebecca PhD4; Bergman, Jacques MD, PhD6
1 University Medical Center Amsterdam, Amsterdam, Noord-Holland, Netherlands;
2 Cancer Center Amsterdam, Amsterdam UMC, University of Amsterdam, Amsterdam, Noord-Holland, Netherlands;
3 Amsterdam UMC, Amsterdam, Noord-Holland, Netherlands;
4 Castle Biosciences, Pittsburgh, PA;
5 Castle Biosciences, Friendswood, TX;
6 Amsterdam University Medical Centres, Amsterdam, Noord-Holland, Netherlands.
Read the full study at the American Journal of Gastroenterology
Abstract
Risk stratification of patients in Barrett’s esophagus (BE) surveillance is largely based on histologic review of biopsies by pathologists, specifically focused on the identification of patients with dysplasia as a surrogate for progression to cancer. However, level of dysplasia is a suboptimal correlate for progression, and new tools to optimize patient risk stratification based on actual progression to high-grade dysplasia (HGD) and esophageal adenocarcinoma (EAC) are needed. A previous study presented at DDW 20222 showed that TissueCypher outperformed 16 general and 14 expert GI pathologists in risk-stratification of BE patients based on outcome to HGD or EAC (progressors). This study evaluated the impact that variability in pathologic diagnosis has on patient care and shows that adding guidance from TissueCypher to the standard of care can improve the consistency of management and increase the percentage of progressors that receive appropriate treatment while reducing the number of non-progressors that are over treated.
The results indicate that TissueCypher may be used to standardize management of BE patients to improve health outcomes:
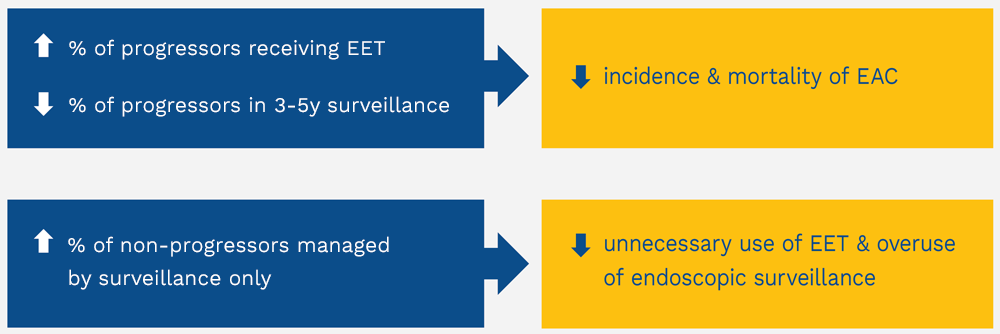

Aims
The aims of this study were to evaluate whether the use of the TissueCypher test can standardize clinical management decisions for BE patients with initial diagnoses of LGD reviewed by various pathologists, and increase the percentage of patients who receive appropriate management in a manner consistent with improved health outcomes.
Methods
The study generated 500 management decision simulations for each of the 154 patients. Each simulation started with a diagnosis from one of the 16 general pathologists. If the diagnosis was low-grade dysplasia (LGD) then confirmation from an expert pathologist in the same country was required, in accordance with guideline recommendations. Next an additional 500 simulations were generated using guidance from the TissueCypher Risk Class. The simulations for each patient were then evaluated based on the patient’s known outcome.
Management Decision Simulation Design
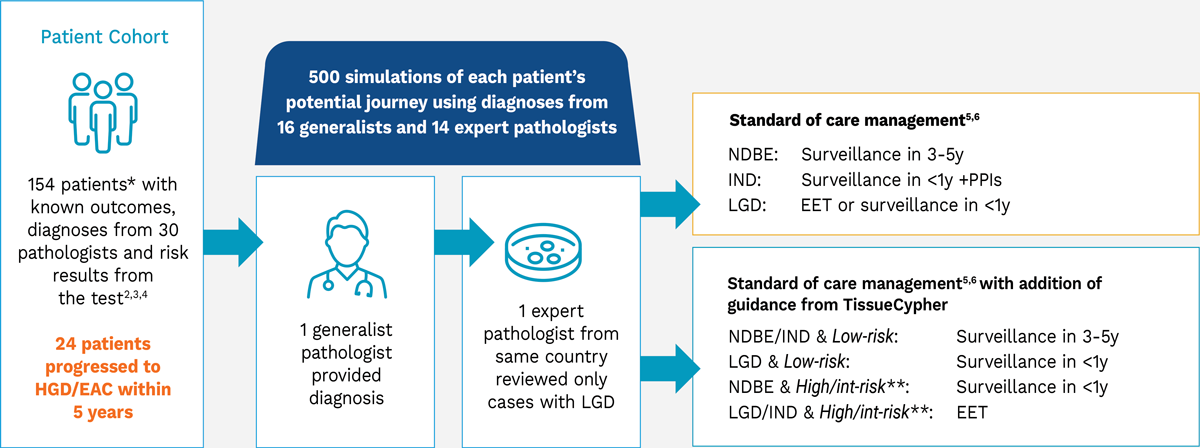
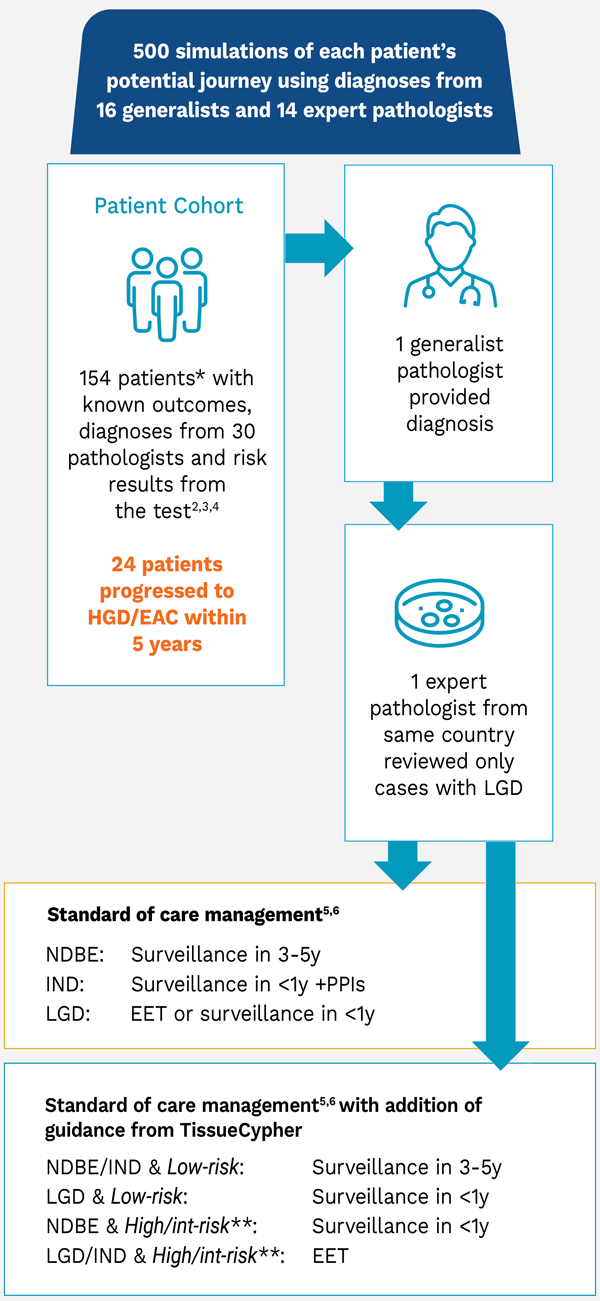
* Patients had an initial community diagnosis of LGD but only 19% were confirmed to be LGD, 13% were downstaged to IND and 68% were doswnstaged to NDBE upon average expert review.2
** NDBE/IND scored High/Int-risk were reviewed by expert pathologist.
Analysis
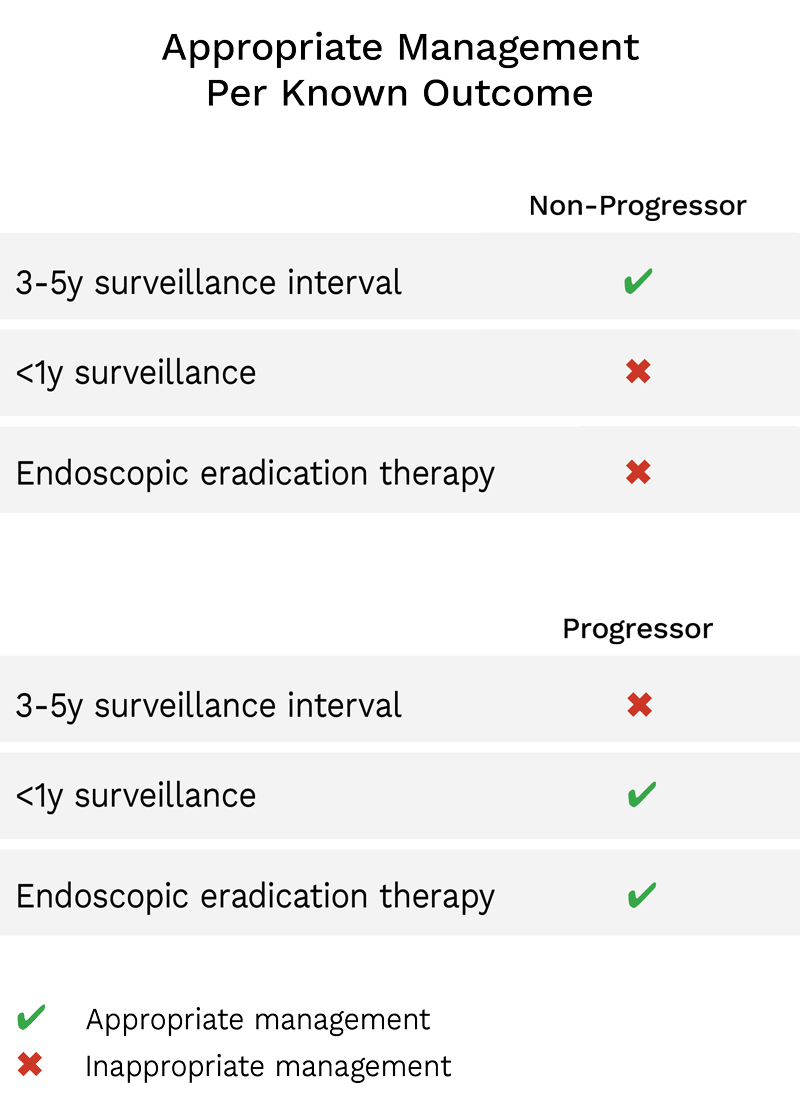
Each patient’s simulations were evaluated based on their known outcome as a progressor or non-progressor. The percentage of appropriate management decisions resulting from the 500 simulations were calculated for each patient. To assess consistency of management decisions, standard deviation was calculated across all 154 patients. In this study appropriate management for a non-progressor was 3-to-5-year surveillance and for a progressor was <1 year surveillance or EET.

Results
TissueCypher guidance clinically and statistically improved the standard of care by increasing the likelihood of appropriate management decisions for all patients and decreasing the variability in management that results from basing care solely on the diagnoses of dysplasia.
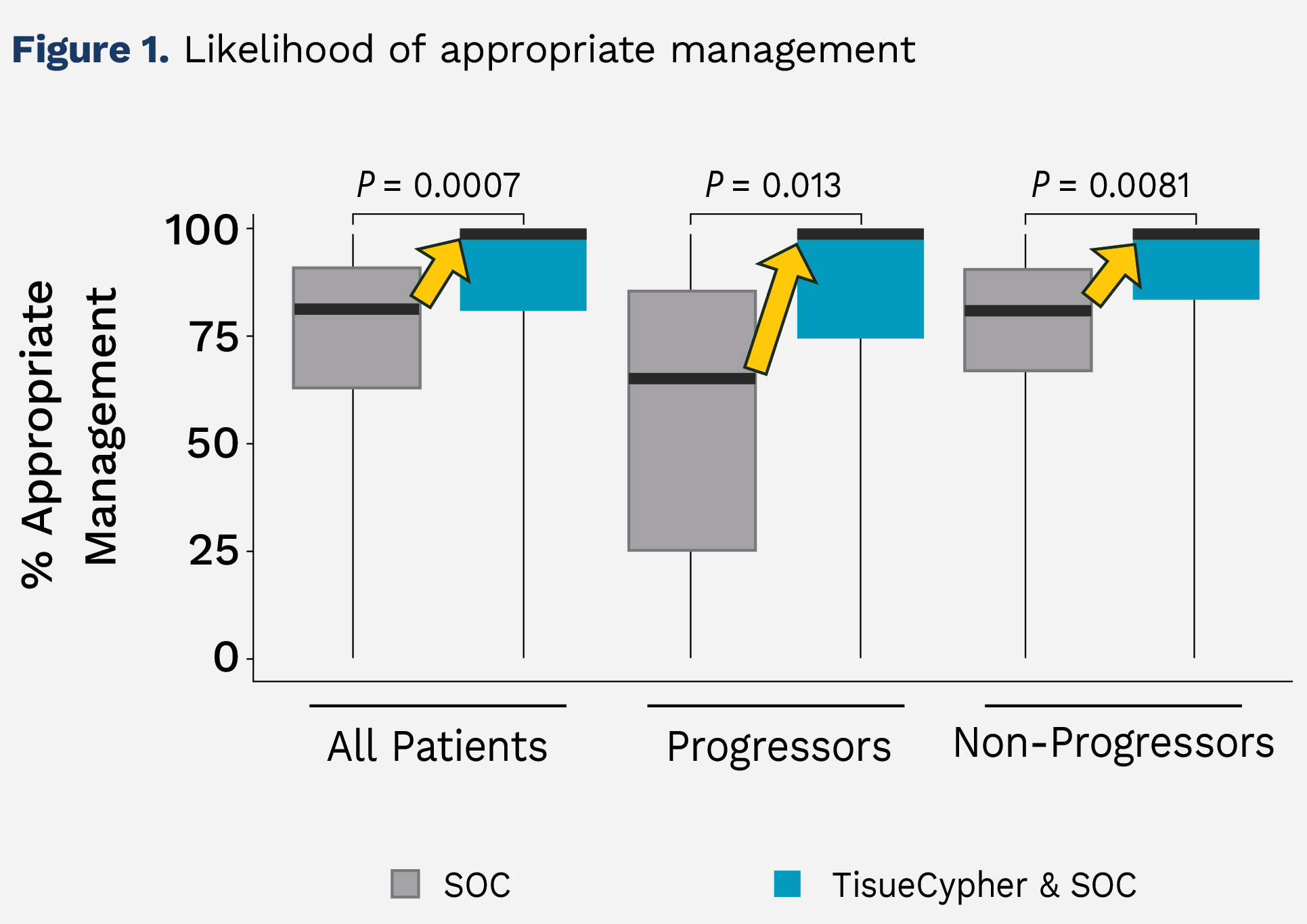
Figure 1 shows the % of appropriate management for all patients was improved by the addition of guidance from TissueCypher to the standard of care (SOC), with the median increasing from 80% to 100%. For progressors there was an increase in the percent receiving EET and a decreased percentage receiving 3-to-5-year surveillance. For non-progressors there was an increased percentage that were managed by 3-to-5-year surveillance.
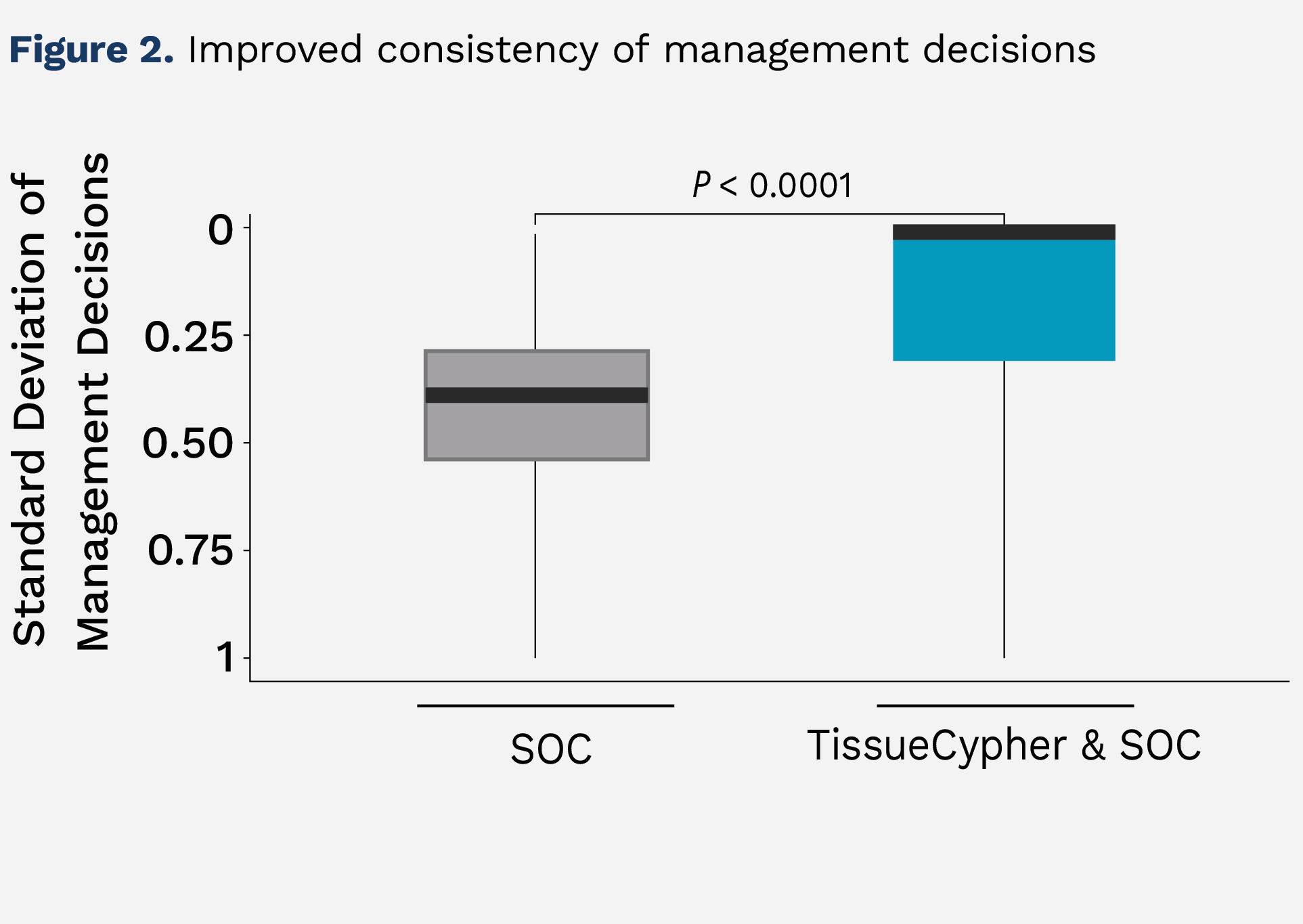
Figure 2 illustrates the improvement in consistency of management across all 500 simulations. For the standard of care (SOC) 7.1% of patients experienced no deviation in management across all 500 simulations. The addition of guidance from TissueCypher increased this number to 57.1% of patients that saw no deviation across all 500 simulations.
References
- Duits LC et al. Am J Gastroenterol. 2023 Jun; [Epub ahead of print]
- Frei NF et al. Am J Gastroenterol. 2022 Oct;117(10S):e269
- Khoshiwal AM et al. Gastroenterology. 2022 May;162(7): S-174
- Phoa KN et al. JAMA. 2014; 311(12): 1209-17
- Frei NF et al. Am J Gastroenterol. 2021 Apr;116(4):675-82
- Shaheen NJ et al. Am J Gastroenterol. 2022 Apr;117(4):559-87
- Muthusamy VR et al. Clin Gastroenterol Hepatol. 2022 Dec;20(12):2696-706.e1
